Now that dental sleep medicine has emerged as one of the fastest-growing areas of dentistry, many dentists have questions about how to implement this mode of treatment into their practice. Here, we answer the most common inquiries we receive from clinicians regarding the treatment of snoring and obstructive sleep apnea (OSA) with oral appliances.
How does dental sleep medicine work?
As an alternative to continuous positive airway pressure (CPAP) therapy, dental sleep medicine involves prescribing a custom-made oral appliance as a means of treating patients who suffer from sleep-related breathing disorders (SRBDs), such as snoring and obstructive sleep apnea. Dental sleep appliances, also known as mandibular advancement devices, work by positioning the lower jaw forward during sleep, thereby activating the muscles and ligaments of the throat to prevent obstruction of the airway and mitigate snoring and sleep-disordered breathing.
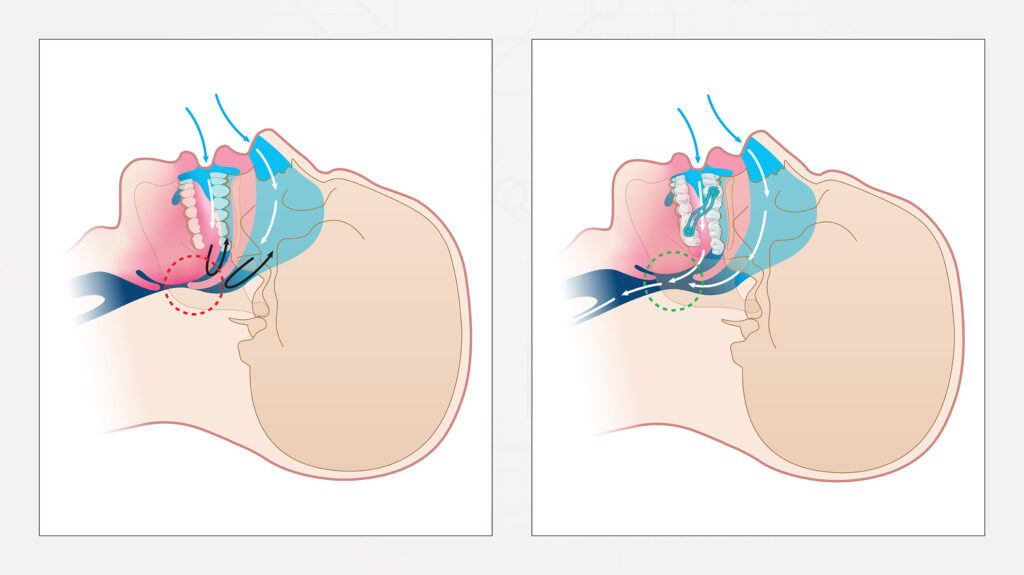
When a patient suffers from sleep-disordered breathing (left), the airway partially collapses, which obstructs airflow, causes snoring and interrupts sleep. When an oral appliance is prescribed as treatment for snoring and obstructive sleep apnea, the mandible is gently positioned forward, thereby creating space in the airway while stimulating the muscles and ligaments of the throat for improved breathing during sleep.
Should I be screening patients for snoring and OSA?
According to the ADA, “dentists are encouraged to screen patients for SRBD as part of a comprehensive medical and dental history.”1 A majority of patients see their dentist more often than their physician, which makes the dentist’s role particularly important in the screening and treatment of snoring and OSA. Oral appliance therapy is a less invasive means of treating SRBDs and is particularly effective for patients who are not able to tolerate CPAP treatment, as noted by the ADA: “Oral appliances, specifically custom-made, titratable devices can improve SRBD in adult patients compared to no therapy or placebo devices. Oral appliance therapy (OAT) can improve OSA in adult patients, especially those who are intolerant of continuous positive airway pressure (CPAP). Dentists are the only health care provider with the knowledge and expertise to provide OAT.”
Basic screening for sleep-disordered breathing involves asking patients about their sleep patterns, reports of snoring from loved ones and the occurrence of daytime sleepiness. In addition, other health problems such as hypertension and obesity are associated with SRDBs, and are cause for additional screening if the patient reports snoring and trouble with sleeping. A simple tool that can be used to screen patients is the STOP Bang questionnaire, which involves asking the patients a series of questions and then calculating a score that classifies the patient as being at low risk, intermediate risk or high risk for OSA. This straightforward tool is available for free to all clinicians at: http://www.stopbang.ca/osa/screening.php.
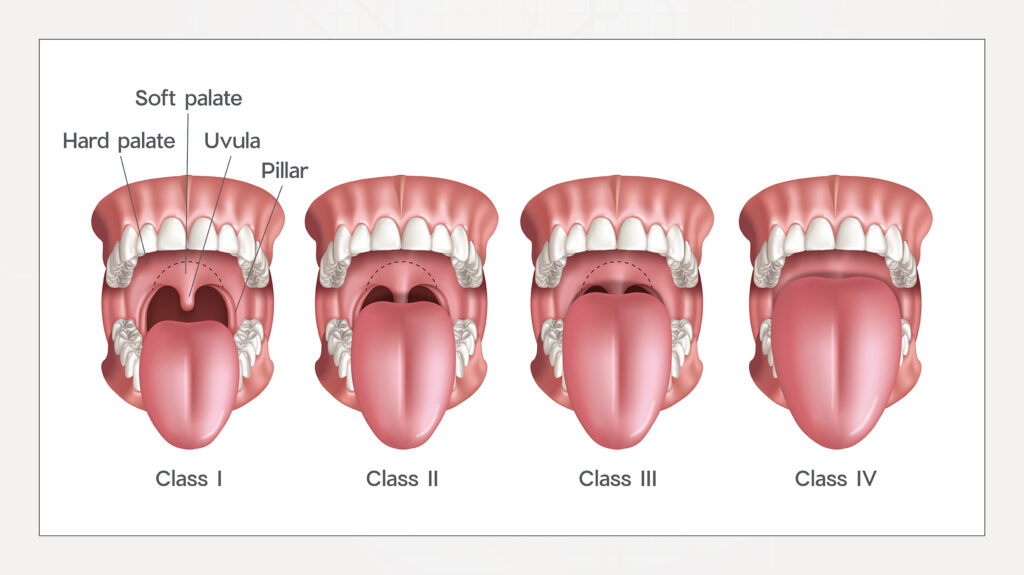
During oral examination of the patient, the throat can also be assessed for signs of restricted airflow, specifically using the Mallampati scoring system. Performing oral airway evaluation during regular screening can go a long way toward identifying patients who suffer from OSA. Using the Mallampati classification system, the patient falls under Class I when the uvula, soft palate and pillars are clearly visible. With Class II, the soft palate and uvula are partially visible. When only the soft palate and base of the uvula are visible, the patient is categorized as Class III. When only the hard palate can be seen, a Class IV determination is made. A Mallampati score of Class III or Class IV is associated with an increased risk of OSA.
How do I prescribe a sleep appliance?
If the patient’s screening determines that they are at risk of OSA, the patient should be referred to a physician for medical management. In the interim, a dental sleep appliance can be prescribed as a provisional form of treatment until a definitive diagnosis is made. This involves informing the patient that the prescribed sleep appliance is for temporary use and instructing them to follow through with their physician. Make sure to document in the patient’s file that your patient understands that the appliance is for provisional use only.
Once the patient has been diagnosed with OSA, they may continue wearing their mandibular advancement device during sleep, and the period of provisional use affords an opportunity for the patient and their physician to gauge the effectiveness of the oral appliance in improving breathing during sleep and reducing snoring. Some patients may continue with oral appliance therapy as their definitive form of treatment, some may eventually move on to CPAP treatment, and some may use a combination of both.
After determining whether a patient is at risk for OSA and obtaining their consent to prescribe an appliance for provisional use, you can submit your case to Riverside Dental Ceramics by downloading and completing an Rx, which should be sent along with full-arch upper and lower impressions, as well as a bite registration.
What types of dental sleep appliances do I have to choose from?

The Silent Nite Sleep Appliance uses connectors to position the jaw forward. The connectors come in various lengths so that the clinician can make a chairside determination of which position is most effective and comfortable for the patient. With more than 400,000 appliances prescribed, the Silent Nite appliance is among the most proven dental solutions for OSA

The EMA oral appliance is a time-tested solution for snoring and OSA that both advances the mandible and opens up the patient’s bite to improve airflow and prevent airway collapse during sleep. With nine different strap lengths and four options for elastic tension, the EMA device affords clinicians a high range of flexibility for advancing the mandible according to the patient’s comfort level.

The dreamTAP appliance holds the lower jaw forward to keep the air way open in a similar manner to that used in the cardiopulmonary resuscitation (CPR) technique. The protrusion of the lower appliance of the device is modified with an adjustment key, making chairside alterations simple.
Why should I consider adding dental sleep appliances to the services I offer patients?
In addition to causing daytime sleepiness, OSA is associated with a range of health problems ranging from high blood pressure, to Type 2 diabetes, to stroke, to coronary heart disease.2 Providing your patients with treatment that reduces snoring and interruptions during sleep can help improve their health and their quality of life, while decreasing drowsiness that can lead to accidents, reduced productivity at work and home, and other negative consequences.
In addition, dental sleep medicine has become a vehicle of practice growth for many dentists across the country. Snoring and OSA are among the health problems in the U.S. that require far more attention, and dentists not only have a role to play in helping patients, but also can expand the services and success of their practices in doing so.
Have more questions or would like some help in getting started with your first sleep appliance case? Call our knowledgeable customer service team at 800-321-9943 for assistance.
EMA is a registered trademark of Frantz Design Inc. dreamTAP is a trademark of Airway Management Inc.
1. American Dental Association [internet]. Chicago: American Dental Association; c2019. The role of dentistry in the treatment of sleep related breathing disorders [cited 2019 Aug 25]. Available from: https://www.ada.org/-/media/project/ada-organization/ada/ada-org/files/resources/research/oral-health-topics/ada_2019_policy_role_of_dentistry_sleep_related_breathing_disorders.pdf?rev=a6b7d4ff667c4325bd1cc402882e0235&hash=1FF15BB2D17D9EA639120DBB78D660E3.
2. Sleep apnea information for clinicians [internet]. Washington, D.C.: American Sleep Apnea Association; c2017 [cited 2018 July 5]. Available from: https://www.sleepapnea.org/learn/sleep-apnea-information-clinicians.